Merit-Based Incentive Payment System (MIPS)
This payment track builds on traditional fee-for-service payments by adjusting them up or down based on a physician’s performance.
CMS recognizes that uncontrollable circumstances may make meeting program requirements difficult and offers exceptions, some of which apply automatically. These exception guidelines may change annually. For the 2025 performance year, two exceptions are available:
- MIPS Extreme and Uncontrollable Circumstances (ECU) Exception – Allows clinicians, groups, and virtual groups to request reweighting of any or all performance categories due to extreme and uncontrollable events.
- MIPS Promoting Interoperability (PI) Hardship Exception – Allows clinicians to request reweighting of the PI category due to issues like insufficient internet, CEHRT vendor problems, or extreme financial distress.
Both applications will be available spring 2025 and are due by 8pm ET on December 31, 2025. Automatic EUC Exception applies to MIPS-eligible clinicians in CMS designated disaster areas, reweighting all four categories to 0% unless data is submitted for two or more. Approved exceptions remove reporting requirements, but physicians may still voluntarily submit data that will be scored if two or more categories are reported.
Major 2025 Changes:
- The weight for all MIPS categories will remain the same as 2024
- Performance threshold
- The minimum performance threshold remains at 75 MIPS points to avoid any penalties
- The exceptional performance bonus was permanently discontinued after the 2024 payment year
- Payment adjustments
- Maximum payment adjustments remain the same at +/- 9%
- This adjustment applies to 2025 Medicare Part B payments for covered professional services
- If a MIPS eligible clinician did not participate in MIPS in 2023, they will receive a negative payment adjustment of –9% in 2025
- Complex Patient Bonus
- CMS continues to offer the complex patient bonus, with a maximum of 10 points added to the final score. MIPS Value Pathways (MVPs)
- MIPS Value Pathways (MVPs)
- Clinicians now have the option to report MIPS through MIPS Value Pathways (MVPs).
- The Data Completeness Threshold is at 75% for calendar year (CY) 24 and CY25
- The 2025 Consumer Assessment of Healthcare Providers and Systems (CAHPS) for the Merit-based Incentive Payment Systems (MIPS) is open until June 30, 2025, at 8:00 PM ET. Groups and APM Entities (other than Shared Savings Program ACOs that choose to report the APP must register because this survey is a required measure under APP. For information on registration and how to register, visit the CAHPS for MIPS Survey page.
- The Merit-based Incentive Payment System (MIPS) Value Pathways (MVPs) registration for the 2025 performance year is open until November 30, 2025, at 8:00 PM ET. Learn more about MVPs, the MVPs finalized for the 2025 performance year, registration information, and more here. Please note that you will have to email your complete registration to QPP@cms.hhs.gov with the subject line MVP Registration.
Please visit our Physician & Practice Timeline to stay on top of these deadlines.
Small and Rural Hospitals
The CMS QPP Small, Underserved, and Rural Support (SURS) initiative ended on February 15, 2022, after five years of direct support. Sign up for the monthly QPP Small Practice Newsletter to receive information tailored to small practices. Read the 2025 MIPS Quick Start Guide for Small Practices to get started with 2025 MIPS participation. Read ACP’s request to extend critical technical program for QPP-SURS.
For performance year 2025, small practices will receive automatic reweighting of the Promoting Interoperability performance category to 0%, whether they choose to participate as an individual or as a group.
You will no longer need to submit a MIPS Promoting Interoperability Performance Category Hardship Exception application to request reweighting in this performance category.
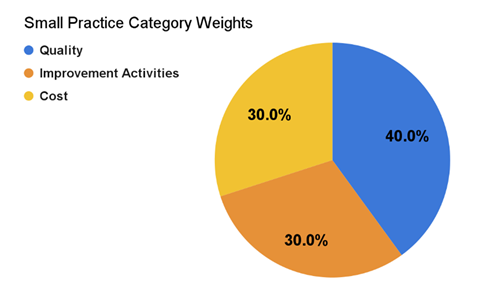
The small practice category weight reflects the finalized performance category reweighting and redistribution policies when the Promoting Interoperability performance category is reweighted. When the cost and Promoting Interoperability performance categories are reweighted, Quality and Improvement Activities will be equally weighted at 50%. When both Quality and Promoting Interoperability performance categories are reweighted, Cost and Improvement Activities will be equally weighted at 50%.
2025 Low Volume Threshold
To be eligible for MIPS, clinicians and practices must exceed the low-volume threshold (LVT) during both segments of the MIPS Determination Period to be eligible for MIPS. Participation in MIPS is required if, in both 12-month segments of the MIPS Determination Period if you:
- Bill more than $90,000 for Medicare Part B covered professional services, and
- See more than 200 Medicare Part B patients, and;
- Provide more than 200 covered professional services to Medicare Part B patients
Segment 1 of the MIPS Determination covers October 1, 2023, until September 30, 2024, and initial eligibility is released on the QPP site in December 2024.
Segment 2 of the MIPS Determination covers October 1, 2024, until September 30, 2025, and final eligibility is released on the QPP site in December 2025.
For more information go to the QPP webpage.
MIPS - Scoring
The MIPS scoring is a composite score of the 4 performance categories:
- Quality - worth 30% of the total. You’ll need to submit collected data for at least 6 quality measures (including one outcome measure or high priority measure in the absence of an applicable outcome measure), or a complete specialty measure set.
- Promoting Interoperability - worth 25% of the total. You must collect data for the required measures in your certified electronic health record technology (CEHRT) for a minimum of 180 continuous days during the calendar year.
- Improvement Activities - worth 15% of the total MIPS score. Beginning in the 2025 performance period, improvement activities won’t be weighted. Improvement activities have a minimum of a continuous 90-day performance period (during calendar year (CY) 2025) unless otherwise stated in the activity description. Each improvement activity must be performed in CY 2025, but multiple improvement activities don’t have to be performed during the same 90-day, or otherwise specified, period.
- Cost - worth 30% of the total score. CMS updated the cost measure scoring methodology to more appropriately incentivize or penalize clinicians with costs above or below national average spending.
Read more on the Calendar Year (CY) 2025 Medicare Physician Fee Schedule (PFS) Final Rule: Quality Payment Program (QPP) Fact Sheet.
MIPS Value Pathway (MVP)
MVPs are similar to MIPS, except all of the measures and activities across all four performance categories will be centered around a particular specialty, condition, or patient population. CMS finalized 6 new MVPs that will be available beginning with the 2025 performance period related to ophthalmology, dermatology, gastroenterology, pulmonology, urology, and surgical care. Additionally, CMS finalized limited modifications to the previously finalized MVPs, including the consolidation of 2 neurology-focused MVPs into a single neurological MVP align MIPS categories, reduce reporting burden, enhance clinical relevance, and create a transition path to APMs.
MVPs remain optional in the 2025 performance year and CMS continues to collaborate with interested parties to refine MVP design.
- ACP Comments on 2025 Physician Fee Schedule, Medicare Shared Savings Program, and Quality Payment Program Final Rule
- ACP comments to CMS for MVP Stakeholder Town Hall
- CMS MVP webpage
MIPS APM Performance Pathway (APP)
In 2021, CMS replaced the “MIPS APM scoring standard” with the new “MIPS APM Performance Pathway (APP).” The APP remains an optional pathway for clinicians that participate in an APM but still participate in MIPS either because: 1) their model does not meet the criteria to be considered an “Advanced APM;” or 2) they fall short of Qualified Advanced APM Participant (QP) Thresholds. Category weights under the APP resemble those under the APM Scoring Standard: Cost: 0%; Promoting Interoperability: 30%; Improvement Activities: 20%; and Quality: 50% (unless reweighting applies). Under the APP, data can be reported at the APM Entity, group, or clinician level. All clinicians under the APP will be scored on the same six quality measures (if available/applicable). For more, read ACP’s comments on the 2025 PFS final rule and access this CMS APP page.
MIPS Resources
From ACP:
- Visit ACP's Improving Medicare page to see the Latest Advocacy Efforts.
From CMS:
- MIPS APM
- Quality Measures
- Promoting Interoperability
- Improvement Activities
- Cost Measures
- For specifics in each category, including scoring, measures (for each reporting method), activities, and specifications for each measure/activity, search the Resource Library.
Have more questions? Email us at policy-regs@acponline.org.

