In the News
We Need a National Strategy to Help Health Workers Recover From the Stress of the Pandemic
By Victor J. Dzau, MD
The Los Angeles Times
In this opinion article in The Los Angeles Times, Dr. Victor Dzau, Chair of the National Academy of Medicine's Action Collaborative on Clinician Well-being and Resilience, argues for a national strategy to measure and respond to clinician burnout.
There is no cavalry riding to the rescue after COVID-19. The pandemic has been the largest, and the longest, strain on the well-being of U.S. health workers in modern history. The solution must match the scale of the challenge.
Health Care Workers Turn to Military Techniques to Deal with Trauma
By Quincy Walters
WBUR.org
Dr. Joshua Morganstein of the Center for the Study of Traumatic Stress believes that the battle buddy programs popularized by the U.S. military are helpful for frontline health care workers during—and after—the COVID-19 pandemic. When Dr. Kerri Palamara wanted to start a support program at Massachusetts General Hospital, she remembered the interview she conducted with Dr. Morganstein as part of the ACP Well-being and Professional Fulfillment initiative and modeled her program after the battle buddy concept. After reading the article, be sure to watch Kerri and Josh's webinar webinar Addressing and Supporting Physician Mental Health during Challenging Times and earn CME!
There are three main areas someone can quickly ask about: How are things at home? How are things at work? And how are you sleeping?
Time to Speak Up: A Graphical Depiction of Psychological Safety in Health Care Teams
By Nour Houbby; Arwa Hagana; Ridhaa Remtulla; Anannya Menon; Kajal Ruparell, BSc; Santhosh Thavarajasingam; and Nivaran Aojula
Annals of Internal Medicine

Hierarchy within health care teams can prevent team members from expressing concerns or new ideas because of fear of negative consequences from seniors. This can subsequently pose a barrier to the provision of care.

A supportive team environment enables individuals to speak up and voice concerns. By positively reacting to a team member speaking up, other team members are likely to feel empowered in the future.
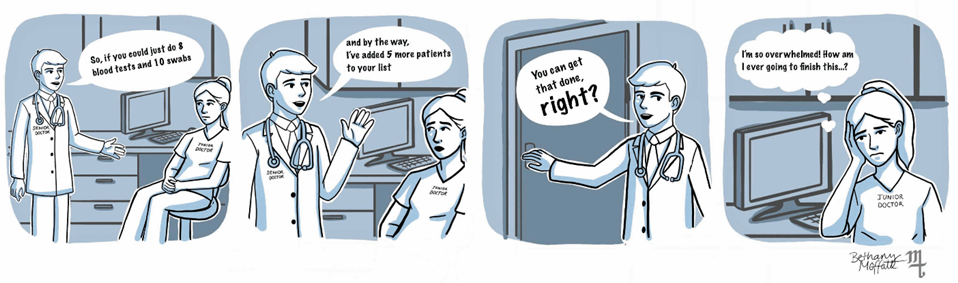
Often, those in more senior positions in health care set unreasonable expectations for more junior members. These expectations can leave individuals feeling overwhelmed and unable to speak up.

New members to the health care team often find themselves isolated from the rest of the team. This can lead to individuals hesitating to voice their opinion despite being able to contribute useful information.
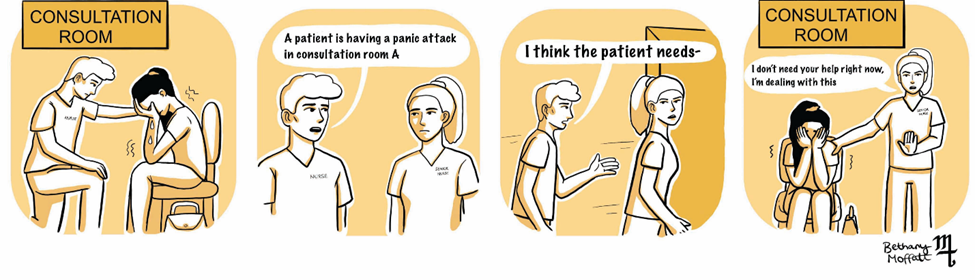
Team leaders may adopt an authoritarian leadership style, failing to acknowledge the contributions of others. This may prevent team members from raising concerns in the future.
Discuss this topic with other ACP members in ACP's Physician Well-being and Professional Fulfillment Forum.

