Rhode Island Governor's Newsletter September 2023

-
In this Issue:
- Governor's Welcome
- Committee Highlights
- Congratulations!!!!
- Mentorship Zone
- From National ACP

Kwame O. Dapaah-Afriyie, MBchB, FACP, ACP Governor
Governor's Welcome
Hello colleagues, I hope you all had an enjoyable summer season. We are at the brink of another season; fall, a favorite of many who enjoy the changing scenery of flowers and other forms of vegetation undergoing color changes and recycling to enrich our ecosystem. This season brings attention to the biologic changes we humans experience and the renewed interest in the concept of ageism.
Ageism and its negative connotations were highlighted at one of the educational sessions at the spring Board of Governors' (BOG) meeting in San Diego. Coined in 1968 by Dr. Robert Butler a Geriatric Psychiatrist, ageism as defined by him is, “discrimination, prejudice, stereotyping based on age.”1 The World Health Organization (WHO) has further expanded this definition as follows, “the stereotypes, prejudice, and definition towards others or ourselves based on age.” As with other forms of discrimination, ageism may be implicit or explicit. In a 2020 National Poll on Healthy Aging, 82% of older Americans reported experiencing ageism.2
Unfortunately, increasing age is invariably negatively associated with inattention and disorientation while ignoring the positive aspects of experience, insight, and wisdom. The longer we live the more we learn, and the more we learn, the more experience we gain and the more insightful we become. Ageism has a negative impact on the physical and mental health of the elderly. A study of a cohort of elderly individuals over a 23-year period revealed that those with a positive self-perception of aging lived 7.5 years longer than those with negative perceptions.
According to WHO estimates, by 2031, I in 6 people in the world will be 60 or more years old. It is expected that this category of people will double in number by 2050.2 These estimates should prompt us to seriously address the notion of ageism and its deleterious effects. We must harness the wisdom of the elderly instead of discounting their invaluable contributions to humanity.
In this post-pandemic era, society (including our medical profession) is dealing with the concepts of ‘Great Resignation’ and ‘Quiet Quitting,” exacting a huge toll on workforce availability and engagement. There is the need for a paradigm shift in dealing with ageism by taking concrete steps to highlight the positive aspects of aging as exemplified by Japan. In this country, the third Monday of September designated “Respect for the Aged day” is observed as a national holiday in honor of the elderly.
In healthcare, ageism has been associated with inattention to needs of the elderly and disparities in care.3 Proposed measures to address the concept of ageism include legislation and policies, however more individual steps are needed. We need to increase our awareness, learn more about ageism to develop action plans to combat its negative effects within our spheres of influence. We need to encourage ourselves and our patients that there is still more in us to offer to society and to stay active so far as we have the requisite physical strength and cognitive ability. Additionally, structured mentorship programs will provide an avenue for professional growth of younger colleagues and medical students.
Finally, addressing ageism will be a major step in combating loneliness and isolation which according to the US Surgeon General, Dr Vivek Murthy, is a crisis which has become one of our generation's greatest challenges.
References
- Butler, R. N. (1969). “Age-ism: Another form of bigotry”. The Gerontologist. 9 (4): 243–246. doi: ) 10.1093/geront/9.4_part_1.243. PMID ) 5366225. S2CID ) 42442342.
- World report on ageing and health. Geneva: World Health Organization; 2015 (https:// apps.who.int/iris/handle/10665/186463, accessed 13 October 2020).
- Leah Nemiroff, We can do better: Addressing ageism against older adults in healthcare, Healthcare Management Forum, 10.1177/08404704221080882, 35, 2, (118-122), (2022).
COMMITTEE HIGHLIGHTS:
(By Mariah Stump. MD. FACP) - WELLNESS COMMITTEE:
The Wellness committee is under the leadership of Wellness Champions, Drs Mariah Stump and Jennifer Jeremiah. The key members of the committee are Dr. Cara Zimmerman, Dr. Lauren Schlanger, Dr Audrey Kupchan and Dr Stephanie Catanese.
The mission of the Wellness Committee is to engage members in events and offerings which support fostering community and connection thereby promoting personal and professional wellness. While we understand that physician wellness stems from more than just participating in activities, and greater system-wide changes in our health care/medical system must be addressed to tackle burnout, we hope that this committee can offer opportunities to build relationships, work on coping skills for stress, or as a way to have fun with colleagues outside the clinical setting!
In order to gauge our members' interest, an ACP wellness survey was given to the chapter in February 2023 which revealed that the chapter has a wide variety of interests for building wellness within the community (see below results from the survey):
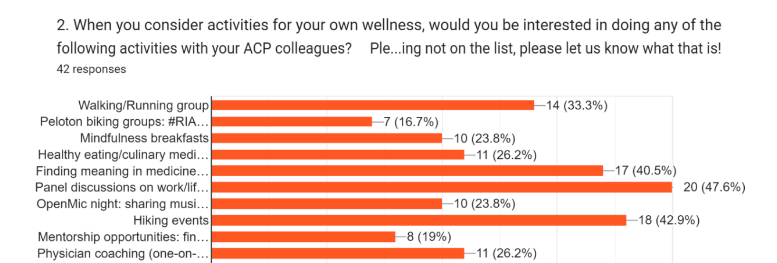
Given these responses, we hope to offer a variety of choices for members to hopefully find what fits them best. Current standing offerings of Wellness activities include: First Wednesday of every month from 8-9 pm EST “Writers Wellness Workshop” in conjunction with the North Carolina ACP chapter. These Narrative Medicine workshops involve a close reading of a poem or short piece of prose and then a reflective writing exercise to prompts associated with themes presented in the work of literature or art. The act of close reading, listening to colleagues as they share their writing reflections (and sharing your own) heightens and strengthens empathy and builds connection. Responses from participants have been very positive! Find the zoom registration link here:
Additional events:
A. A membership presence at the “Suicide in Healthcare and Science: We're Talking About It” day at Alpert Medical School on 9/20/23.
To Register, visit: go.brown.edu/NPSADay CME credit for physicians is available.
B. A team presence is needed for Dr Tom Olilla's annual Bike fundraiser “Tour de Rhody” to support the Brown University Oncology Research Group (BrUOG) and is hosted by the Lifespan Cancer Institute. Sign up today .
Finally, one of our priorities this year are to destigmatize physicians seeking mental health services and ensuring that questions pertaining to this are taken off the current medical licensure applications in the state of Rhode Island. This is very detrimental to physician wellbeing and is often a deterrent for physicians to seek the mental health care that they need. If you are interested in helping with this effort, please contact me.
Congratulations !!!!
To our Fellows of the College:
New fellows: Dr. Kevin K. Chen, Dr. Denise Fernandes, Dr. Matthew Lynch, and Dr. Jessica Murphy
Our Chapter once again received a Gold Chapter Excellence Award for our activities in 2023. Thanks to Kelly McGarry, Committee Chairs, Council members and all of you for your insight, participation, and assistance.
Mentorship Zone
What are we learning? Who are we learning from? Who are we transferring insights to?
Iron sharpens iron, so one person sharpens another.
The one who waters will also be watered.

Tom Bledsoe, one of our former Governors, share some insights with us in the section :
Brief background: Tom Bledsoe MD, MACP. Brown/Dartmouth Medical Schools 1984-1988, Internal Medicine Primary Care at Rhode Island Hospital 1988-1991, last solo Chief Resident at RIH 1991-1992 (first year of admission caps for incoming interns!) General Internal Medicine practice since then. Former RI ACP Governor, former ACP Regent and past chair of ACP's Ethics Professionalism and Human Rights and Awards Committees, Chair of Rhode Island Hospital Ethics Committee, current (until September) President of the Rhode Island Medical Society.
1. Why did you choose to specialize in internal medicine?
Despite narrowing my preferences to surgery and psychiatry (!) before arriving at medical school, it was the science and scientific reasoning of internal medicine, the challenge of making sense of the varied presentations of a world of diseases in a world of individual persons who got sick that drew me in. I think part of me also saw general internal medicine as the epitome of “doctoring”, a personal and professional ideal I could embrace. (Interestingly, the idea of being someone's doctor potentially for the rest of their life was the most daunting concern about GIM.)
2. What are the 2-3 major factors that have helped you in this profession?
a. I've always tried to “mix it up” a bit in my days and weeks. For many years, I attended on the wards as a service attending for three or four months per year as well as precepting in medical clinic or in my office, taking pleasure in both the mentoring and in the challenge of trying to stay a few steps ahead of some very smart medical students and residents while watching their incredible personal and professional growth.
b. I always had a background interest in medical ethics and when the opportunity arose to both get more professional training and help the ethics committee, I jumped at both. As I wanted to gain more experience in this area, I made a resolution early on to never say no to a request for help with ethics problems and gradually became a resource for the community in this area. This has nicely complemented clinical work.
c. I've gradually come to see that physician participation in the system (within medical structures but also more broadly and politically) is the only way that things will improve. Our input is critical but so is collaboration. That led me to work with Rhode Island's primary care redesign project, the Care Transformation Collaborative, the Rhode Island Chapter of the ACP and eventually to my work on the Board of Regents and the Medical Society.
3. What has kept you in this profession amid the challenges?
a. I have a large practice and still see many patients I met in the first few months of my professional career. Seeing them daily, knowing them “in sickness and in health” over the years and being there for them when things are complicated is immensely satisfying.
b. I have learned new things every day of my career, the intellectual challenges and acquisition of new knowledge pulls me forward. Being a general internal medicine specialist in a robust medical community also makes it possible to get help when I need it.
c. Seeing new challenges in the practice environment and knowing both that change is difficult but also that change is possible both pushes and pulls me toward active involvement in how those changes are envisioned and enacted
From National ACP
Listed below are the resolutions to be reviewed at the Fall BOG meeting. We will be discussing these at the next Governor's council meeting on September 20.
Kindly send any input you have to me, Roni Phipps, our executive director, or to a council member.
1-F23. Allocating Resources to Create Awareness of the CPT and RUC Process (Sponsor: Delaware Chapter)
Resolution 2-F23. Extending National ACP Efforts to Improve the Preauthorization Process (Sponsor: District of Columbia Chapter)
Resolution 3-F23. Improving the Effectiveness of EMR Notes by Discouraging the Use of “Cut and Paste” in Progress Notes [ACCEPTED AS REAFFIRMATION -- NO DEBATE] (Sponsor: District of Columbia Chapter)
Resolution 4-F23. Developing Policy to Support Hospital-at-Home Care Models (Sponsor: Wisconsin Chapter; Co-sponsors: Maryland and New York Chapters)
Resolution 5-F23. Educating Physicians about Resources to Aid in Reducing Office Staff Shortages (Sponsor: District of Columbia Chapter)
Resolution 6-F23. Developing Resources to Educate ACP Members about Fertility and Family Planning (Sponsor: Council of Resident/Fellow Members; Co-sponsors: Council of Early Career Physicians and Council of Student Members)
Resolution 7-F23. Revising the Policy of Cancellation Fees for ABIM Certification Exams (Sponsor: Michigan Chapter)
Resolution 8-F23. Phasing Out Pharmaceutical and Other Industry Sponsorship of ACP's Annual Internal Medicine Meeting (Sponsor: Washington Chapter.

