This toolkit includes team-based resources that can help physicians, their teams, and their patients optimize team-based care in a pandemic/post-pandemic setting.
Funding for the COVID-19 Recovery Team-Based Care Toolkit was made possible by Pfizer, Inc.
Table of Contents
- What Is Team-Based Care?
- Steps to Optimal Team Based Care Framework
- Discussing Team-Based Care with Patients
- Effectiveness of Team-Based Care in a Pandemic
- Separate Triage Settings
- Safely Resuming Care
- Managing Transitions of Care for Post-Acute COVID Patients
- Using Telehealth to Manage High-Risk Chronic Conditions
- Informing Patients about Changes in Practice
- Sustaining Teams and Positive Changes
- Emerging Models of Team-Based Care

What Is Team-Based Care?
Team-based model of care strives to meet patient needs and preferences by actively engaging patients as full participants in their care, while encouraging all health care professionals to function to the full extent of their education, certification, and experience.
- Health care teams are defined as two or more health care professionals who work collaboratively with patients and their caregivers to accomplish shared goals.
- A health care team may involve a wide range of team members in various settings.
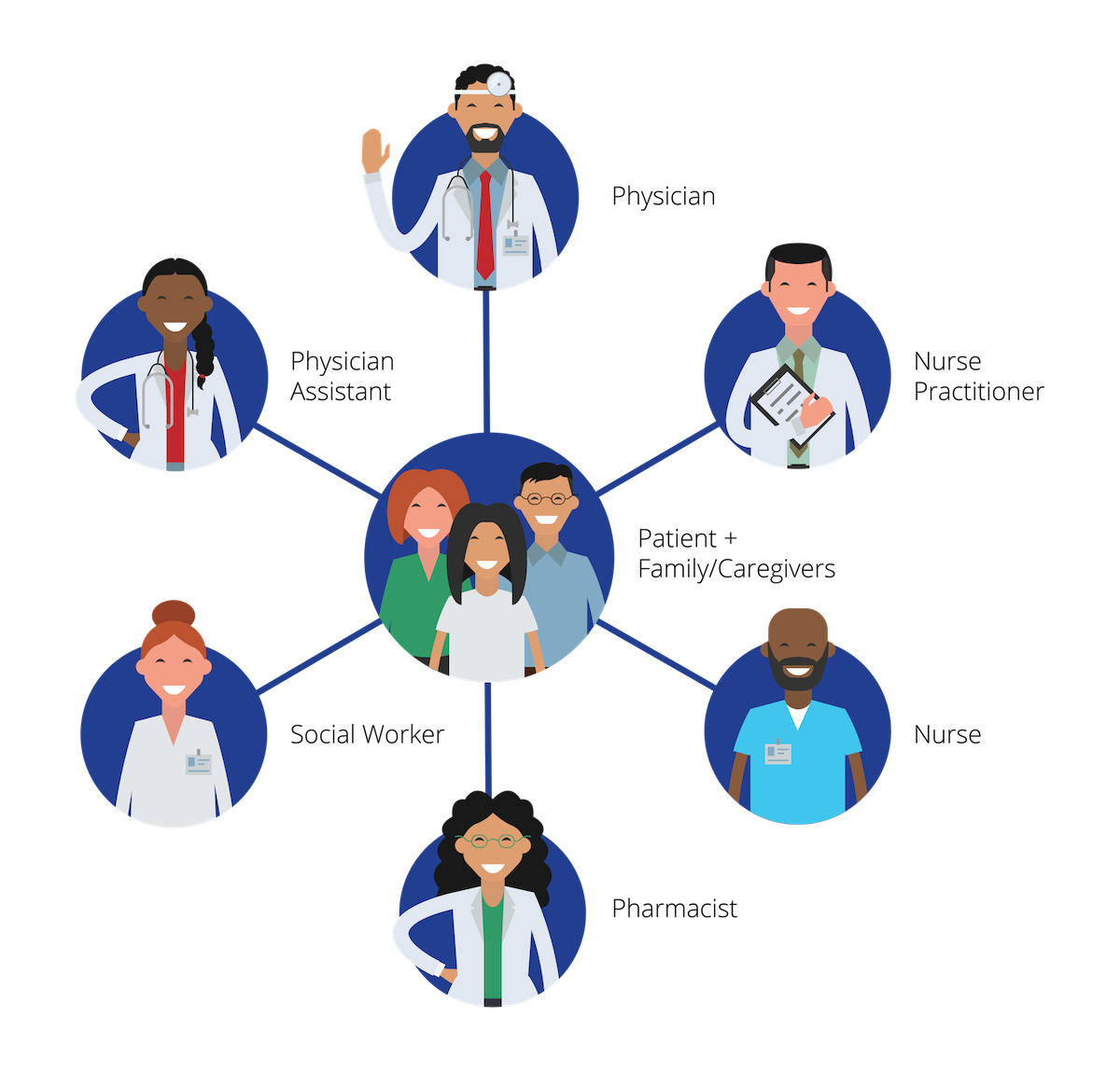
- Potential members include physicians, nurses, pharmacists, social workers, trainees, patients and their families, and others identified as persons necessary to help achieve shared goals.
Resources
Access these resources to help you define the team and understand general principals behind team-based care:
- A New Approach to Making Your Doctor-Team More Productive - This article from the AAFP gives tips on how to create a productive clinical team. It explains how with proper training and delegation, your team can see more patients, deliver better care, and increase patient and staff satisfaction.
- Keys to High Functioning Office Teams - This article from the AAFP focuses on tips including hiring more nurses or medical assistants and more effectively distributing work and responsibilities to create high functioning teams to revolutionize your practice.

Steps to Optimal Team-Based Care Framework
- Foster mutual trust, physical, and psychological safety.
- Clarify roles and expectations.
- Practice effective communication.
- Track a set of shared measurable goals.
Resources
Access these resources to help build this framework and ensure clinical and administrative systems support team members in their defined work:
- IOM Core Principles & Values of Effective Team-Based Health Care – Developed by participants from the IOM's Best Practices Innovation Collaborative, this discussion paper identifies key findings from health care literature and uses interviews with eleven teams located across the United States to clarify how these factors shape effective team-based care.
- Huddles: Improve Office Efficiency in Mere Minutes - Daily gatherings of your care team can help you meet daily challenges. The American Academy of Family Physicians posted this article to help physicians identify when and how to conduct a team huddle.

Discussing Team-Based Care with Patients
Patients, families, and other caregivers need a clear understanding of the roles of the interprofessional care team with explanations of which role will serve which purpose in their care. The health care team should provide information to patients, families, and other caregivers so they can make informed healthcare decisions in partnership with their care team.
Resources
The following resources can help patients understand the different roles that make up the interprofessional health care team and how they might interact with each:
- Who's Who on the Healthcare Team: An Interdisciplinary Approach - This article provides a brief introduction to the educational background and role of the different professionals a patient might typically encounter in a hospital.
- Your Health Care Team - This article provides a brief description of the roles of the different professionals a patient might typically encounter in a hospital.

Effectiveness of Team-Based Care in a Pandemic
The unprecedented global health crisis of the 2019 coronavirus outbreak has presented a unique opportunity for mass mobilization towards team-based care and collaboration in the health care space. In the past, teamwork in health care has been limited by power hierarchies. COVID-19 has leveled the playing field in some ways; no one has experience treating a public health emergency of this magnitude. Doctors, nurses, advanced practice practitioners, and other key figures on the frontline need to collaborate, communicate, innovate, problem solve, remove silos, and recognize that everyone is on the same team in a collective effort against the virus for the betterment of the patient.
(citation: https://patientengagementhit.com/features/how-coronavirus-sparked-industry-collaboration-team-based-care)
Resources
Access these resources on harnessing the power of team-based care and providing effective care in a pandemic and post-pandemic setting:
- COVID-19 communication: Refining team-based care in a time of crisis - This article includes practical tips and best practice examples from a health center in Wisconsin on how they evolved team-based care for pandemic care.
- Supporting The Non-Traditional Health Care Workforce: Community Health Workers and Promoters – This resource outlines how to support a non-traditional workforce of community health care workers and promoters who provide an essential role in supporting patients with complex medical and social needs.
- Reducing Health and Health Care Disparities: Implementation Lessons and Best Practices for Health Care Organizations – This article includes concrete recommendations that health care organizations can use to improve the quality of their health care delivery systems and implement interventions to address inequities in patient care and outcomes.

Separate Triage Settings
Many members of the healthcare team will have a role to play in in assuring that the patient triage process is safe and efficient. It is essential that potential COVID-19 patients be triaged separately from those with non-COVID concerns in separate settings to reduce infection.
Resources
These resources can help your practice set up and manage separate triage areas.
- COVID-19: An ACP Physician's Guide - This online learning activity is free to the public and provides a clinical overview of infection control and patient care guidance. Up to 10 CME credits are free to ACP members and provided at a nominal fee to non-members.
- COVID-19 Telemedicine Risk Tier Assessment – This chart can help practices assess how to determine a patient's COVID-19 risk during a telemedicine visit.
- Scripts for COVID-19 telephone triage – Use this script and accompanying decision algorithm and messages from the CDC when assessing possible COVID-19 patients over the phone.

Safely Resuming Care
Safely resuming care during and post-COVID will require the effort of the entire team from front-office staff to community partners. It is essential to outline the job descriptions and roles of various team members (including clinic administrators) and develop appropriate workflows, checklists, and other documentation to ensure protocols are followed appropriately.
Resources
Access these practical resources to help your practice safely resume care.
- Innovative Staffing Models - Implementing innovative staffing models will be key for your practice's COVID-19 recovery plan. Innovative staffing models help to ensure the safety of your office staff, offer flexible options for your staff in the time of a pandemic, help to identify core functions that can be done in the office versus remotely, and help you to prepare in the event of staff shortages due to staff or family member illness.
- Sample Job Descriptions – This site includes job descriptions for contact tracer, contact tracing supervisor, case investigator, and care resource coordinator.
- Sample Job Descriptions – This site includes opportunities and job descriptions from the University of Pennsylvania's Community Health Worker Program (IMPaCT).
- Workflow modifications to ensure patient and clinician safety - Workflows and procedures should be evaluated for needed modifications to ensure the safety of patients and office staff by limiting contact and physical interactions between clinical and office staff and patients. Workflows should also maximize the value of the in-person visit. This resource provides practical suggestions to adjust your office workflows to ensure patient and clinician safety.
- Preparing your office for re-opening – ambulatory infection control checklist - Your practice will need to implement infection control procedures to reduce risk of transmission from known or suspected COVID patients as well as asymptomatic or pre-symptomatic carriers. This checklist is designed to help your practice reduce risk and guard the safety of your patients and clinical and office staff.
- COVID-19: Team and Human Factors to Improve Safety – This article discusses how human weaknesses impact individual clinicians and care teams in ways that could degrade patient safety, reduce quality of care, and increase risk for both patients with COVID-19 and the staff that care for them.
- COVID-19 Contact Tracer Job Description Template – This CDC template includes an introduction to case investigation, a position summary, essential functions, work requirements, and qualifications for a typical contact tracer job.

Managing Transitions of Care for Post-Acute COVID Patients
As patients recover from acute COVID-19 infection, it is imperative that their care team works collaboratively to manage the various transitions of care they will face as they move from the hospital to home or to a long-term care facility.
Resources
Access these resources to help manage transitions of care for patients moving from the hospital to home or to a long-term care facility.
- CDC Interim Guidance on Discontinuation of Transmission-Based Precautions and Disposition of Patients with COVID-19 - Decisions on discharge to home or a long-term healthcare facility should be made in consultation with state public health departments and should consider both the home's suitability for and the patient's ability to adhere to home isolation recommendations.
- Hospital to Post-Acute Care Transfer Form - This tool from the Michigan Department of Health and Human Services can help facilitate communication during the transition from the hospital to the post-acute care setting.
- COVID-19 Lessons from the Front Line: Transitions and Care of the Post-Discharge Patient – This video (41 min.) includes lessons learned from frontline clinicians at Emory University and UCLA. Topics include team workflow examples, post-hospital clinical course experiences, and logistical tips.
- Transition-of-Care (TOC) Pharmacists Fill Gaps During COVID-19 - Many health systems have TOC pharmacists who can help fill such care gaps in patients with diabetes, heart failure, and other chronic diseases. But doing so while tackling a new virus that experts still do not fully understand presents a new challenge—one that pharmacists are rising to meet.

Using Telehealth to Manage High-Risk Chronic Conditions
Health care teams can use telehealth to safely and effectively manage patient populations with chronic conditions during the pandemic understanding that there is still a need for in-person care. Access these resources designed to help teams optimize telehealth and identify where and how patients with chronic conditions can safely receive in person care when necessary.
Resources
Access these resources on optimizing telehealth, remote patient monitoring, and identifying where and how patients should receive in-person care:
- ACP Telemedicine Guide – This online CME program provides crucial information for those looking to begin or expand the use of telemedicine. It includes guidance about coding and using telehealth. The module offers 2 CME credits, free to ACP members.
- ACP Telehealth Guidance and Resources – This ACP resource provides information needed to provide and bill for technology-enabled care, including video visits, telephone visits, virtual check-ins, online digital E&M, and remote patient monitoring.
- A Complete Guide to Using Telemedicine in Your Practice - This guide to seeing patients virtually covers different types of visits, choosing the right tools, implementation, training, reimbursements, patient adoption, patient satisfaction, and tracking metrics of success.
- Virtual Visit Patient Guide – This PDF from the National Health Information Technology Family Advisory Council helps patients understand the purposes of virtual visits and provides an appointment checklist.
- Shift to Telemedicine Doesn't Diminish Value of Team-based Care – This article from the AMA provides links to COVID-19 resources for practices and advice from physicians.
- CDC Framework for Healthcare Systems Providing Non-COVID Clinical Care during the Pandemic - This resource provides healthcare systems with a framework to deliver non-COVID-19 health care during the COVID-19 pandemic.
- Telemedicine Relationship-Centered Communication Skills – This document shares examples of relationship-centered communication skills for communicating in healthcare encounters during a challenging time.
- Virtual Visit Patient Guide: The PFA Network’s National Health Information Technology (HIT) Patient Family Advisory Council developed this one-page guide to encourage patients to have virtual visits with their providers when possible during the pandemic. The guide is available in English and Spanish.

Informing Patients about Changes in Practice
The healthcare team should communicate with patients, families, and other caregivers about changes they are making in the practice to promote transparency and ensure patients feel safe and confident in returning to care.
Resources
Use these resources to inform and educate patients and their caregivers about changes they may encounter when returning for care.
- Infographic on where and when to seek non-COVID care during the pandemic - This infographic provides color-coded and simplified guidance for patients regarding where and when to seek non-COVID care during the pandemic.
- Template for practice communication to patients about reopening or resuming care - This communication template is available for practices to personalize into a communication with their patients about office re-opening plans.
- FAQs for patients on seeking non-COVID care during the pandemic - This document is designed for physicians to share with their patients. It addresses common questions regarding seeking non-COVID care during the pandemic, explains the importance of resuming care, clarifies differences between in-person versus telemedicine visits, addresses safety precautions, and answers other personal and logistical concerns patients may have about seeking care at this time.
- Patient and Family Engagement During a Pandemic (webinar recording – 60 min.) – This webinar from PFCC Partners talks about patient and family engagement during a pandemic and how health care providers, patients, and families have engaged in innovative ways in the face of COVID-19.
- Patient Messaging during COVID-19 Slide Set (webinar slides) - This webinar addresses unique needs during COVID-19, information that should be shared with patients, and how to make communication a two-way street especially with the emergence of hybrid care.
- Patient Priorities Care conversation guide - Patient Priorities Care (PPC) is a structure for having conversations with older patient about what matters most to them, namely their health values, outcome goals, healthcare preferences, and making collaborative healthcare decisions. PPC has developed this conversation guide for conducting effective telehealth clinic visits based on the principles of Patient Priorities Care (PPC).

Sustaining Teams and Positive Changes
Psychological and physical safety is paramount. A lack of PPE and job loss are negatives that have come from COVID-19. In addition, physicians and their team members may feel resistant to integrating team-based care models. However, these models can help reduce burnout and sustain teams in the long term. In addition to acknowledging challenges, it is important to focus on the bright spots that have come out of the coronavirus pandemic (e.g., telehealth, pay/reimbursement), what has worked well, and how to incorporate those into the workflows post-COVID.
Resources
These resources address how team-based care can reduce burnout and how to sustain team-based care models in the long term.
- ACP's Well-being and Professional Fulfillment Resources – These resources from ACP can help physicians and their teams reduce burnout and find ways to enhance professional fulfillment and well-being.
- Team-based Care and Flexible, Adaptable Leadership - Effective team-based care and leadership support is critical to helping your practice manage the unprecedented challenges of the COVID-19 pandemic. This resource provides a menu of recommendations to help you develop a plan for effective team-based communication and leadership in your practice.
- Addressing Postpandemic Clinician Mental Health - The COVID-19 pandemic presents unique challenges that surpass those of previous pandemics, suggesting a significant mental health toll on clinicians. Long-term, proactive individual, organizational, and societal infrastructures for clinician mental health support are needed to mitigate the psychological costs of providing care during the COVID-19 pandemic.
- Pandemic Workforce Well-Being: A Comprehensive Toolkit for Supporting Our Own During COVID-19 – This toolkit from Mount Sinai covers a variety of approaches to addressing the basic, psychosocial, and mental health needs of health care workers on the front lines of the pandemic.
- Implementing Optimal Team-Based Care to Reduce Clinician Burnout – This article from the National Academy of Medicine discusses features of successful health care teams, reviews existing evidence linking high-functioning teams to increased clinician well-being, and recommends strategies to overcome barriers to optimal team-based care.

Emerging Models of Team-Based Care
Real-life examples of successful team-based care during COVID-19 are starting to emerge from practices around the country. These examples showcase ways in which team-based care involving nurse practitioners, physicians' assistants, pharmacists, and others are working together with patients and caregivers together during the pandemic.
Resources
- How One Health System is Transforming in Response to COVID-19 - This article discusses the four stages of the Geisinger Health System's response to the pandemic and argues that transforming care delivery and payment systems as a result of the pandemic can fundamentally improve health care for our nation.
- How Banner Health Redefined Patient Experience with Patient Safety - This article discusses how Banner Health used digital patient intake to decrease waiting room foot traffic and promote patient safety as critical to the patient experience.
- Building Hope: HMS faculty central to creation, operation of Boston's post-acute COVID-19 hospital – This article discusses how team work helped together to set up a post-acute COVID-19 hospital in Boston.

